
Introduction
5.8 million Americans delay necessary medical care each year because they lack transportation — and for healthcare providers, that gap lands squarely in their lap.
Non-emergency medical transport (NEMT) is the structured process hospitals, skilled nursing facilities (SNFs), dialysis centers, and outpatient clinics use to move medically stable patients safely to and from scheduled appointments. Unlike emergency services, NEMT serves patients who need assistance due to mobility limitations, chronic conditions, or post-acute care needs — but require no emergency intervention during transit.
Most NEMT coverage focuses on the patient experience. But healthcare providers carry the operational weight: assessing need, documenting medical necessity, coordinating with transport companies, and protecting continuity of care.
When that coordination breaks down, the consequences are direct: missed appointments, delayed treatment, and avoidable readmissions. Patients who miss care due to transportation barriers incur 111% higher medical expenses than those who don't — a cost that ultimately cycles back to providers and the broader system.
TL;DR
- NEMT is scheduled medical transportation for patients who cannot drive or use public transit safely; healthcare providers initiate and coordinate it
- Providers assess functional limitations and match patients to the right transport type: ambulatory, wheelchair, or stretcher
- Most NEMT requests require documented medical necessity through a Provider Certification Statement (PCS)
- Medicaid covers NEMT as a mandatory benefit; Medicare and private insurance coverage is more limited
- Choosing reliable, licensed NEMT partners directly affects patient outcomes and facility performance
What Is Non-Emergency Medical Transport?
NEMT is a regulated transportation service that moves medically stable patients to and from scheduled healthcare appointments when they cannot safely drive or use standard public transit—it is not an ambulance service. The distinction matters for both clinical and billing purposes.
NEMT differs from emergency medical services (EMS) in several key ways. It is pre-scheduled and does not involve on-board emergency intervention or medical monitoring. The service covers routine, ongoing, or post-acute care needs — not life-threatening situations. Patients require transportation assistance due to mobility limitations, not medical instability.
Vehicle Types Used in NEMT
Healthcare providers order from three primary vehicle categories when arranging NEMT:
| Vehicle Type | Patient Eligibility | Key Requirement |
|---|---|---|
| Ambulatory/Sedan | Walks independently or with a cane/walker | Can transfer to a standard car seat; no specialized equipment needed |
| Wheelchair-Accessible Van | Uses a wheelchair; cannot transfer to a car seat | Lift- or ramp-equipped with securement systems; patient stays in wheelchair |
| Stretcher/Litter Van | Cannot sit upright for the trip; must travel reclined or supine | Medically stable but requires a stretcher — distinct from BLS ambulance transport |

Sedan transport is the most cost-effective tier. Stretcher transport is the most frequently misclassified — patients using this service are stable and need no clinical monitoring, which is what separates it from an ambulance.
Why Healthcare Providers Rely on NEMT
Transportation barriers are among the leading causes of missed medical appointments nationwide. An estimated 5.8 million people in the United States delayed medical care in 2017 because they did not have transportation, and a 2024 CDC report found that 5.7% of U.S. adults lacked reliable transportation for daily living in 2022. The clinical and operational impact on healthcare facilities is direct: no-shows disrupt scheduling and revenue, while missed follow-up appointments increase readmission risk. For heart failure patients, transportation difficulties and other social risk factors increase the odds of 30-day readmission by 62%.
Healthcare providers arrange NEMT most frequently for these patient populations:
- Seniors who no longer drive or lack family support for transportation
- Dialysis patients requiring 2–3 trips per week—nearly 500,000 U.S. patients receive in-center hemodialysis, requiring over 70 million roundtrips annually
- Hospital or SNF discharge patients transitioning home or to another facility
- Individuals with physical or cognitive disabilities who cannot safely use public transit
- Post-surgical patients who are medically cleared for discharge but cannot operate a vehicle
NEMT as a Readmission Prevention Tool
Hospitals and post-acute facilities increasingly use NEMT to reduce preventable readmissions. Patients who miss follow-up appointments are significantly more likely to return to the ER. NEMT supports continuity of care after discharge by ensuring patients attend critical post-acute appointments—wound checks, medication management visits, cardiac or pulmonary rehabilitation, and primary care follow-ups.
Medicaid's Mandatory NEMT Benefit
For Medicaid-covered patients, federal law requires state programs to provide NEMT as a covered benefit under 42 CFR § 431.53 when no other transportation is available. The Consolidated Appropriations Act, 2021 formally codified this requirement into federal statute. Healthcare providers who understand this requirement can advocate for qualifying patients rather than allowing appointments to fall through. However, despite its availability, less than 5% of Medicaid beneficiaries utilize NEMT, often due to complex scheduling requirements and lack of awareness.
The "Extension of the Facility" Model
That scheduling complexity and low awareness gap is exactly where the facility-vendor relationship becomes critical. Professional NEMT providers function as an arm of the healthcare team when they hold approved vendor status with facilities. Their punctuality, driver training, and safety standards directly reflect on the facility's care quality and patient experience.
AllCare Medical Transport, for example, operates 24/7 with PASS-certified drivers for wheelchair and stretcher transport, full Florida licensing, and mandatory background checks—built specifically to meet the standards facilities require from an approved transport partner.
How Healthcare Providers Coordinate NEMT: Step by Step
Coordination typically moves through five stages—assessment, documentation, scheduling, transport execution, and follow-up—each requiring specific actions from clinical and administrative staff.
Step 1: Assess the Patient's Transport Need
The first step is clinical assessment. Providers must evaluate the patient's functional limitations to determine whether they qualify for NEMT and what level of service is required. Key questions include:
- Can the patient walk independently or with minimal assistance? (ambulatory)
- Does the patient require a wheelchair and cannot transfer to a car seat? (wheelchair-accessible)
- Must the patient travel lying down due to medical condition or comfort? (stretcher)
This assessment must be documented and drives all subsequent decisions, including insurance authorization and vehicle assignment.
Step 2: Document Medical Necessity
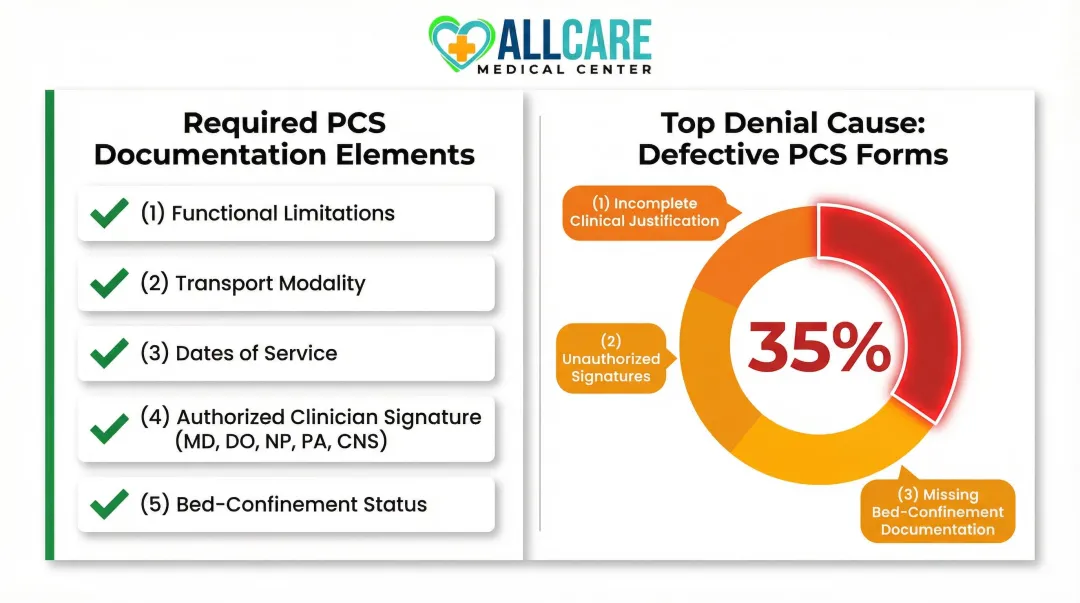
Most NEMT arrangements—especially for Medicaid patients—require a Provider Certification Statement (PCS) or equivalent authorization form. The PCS must be completed by a licensed practitioner (physician, PA, NP, or other qualified provider) and must document:
- The patient's functional limitations that prevent safe use of personal or public transportation
- The required transport modality (ambulatory, wheelchair, or stretcher)
- The dates of service needed
Approximately 35% of all prior authorization denials for NEMT are due to missing or defective PCS forms. Common errors include incomplete clinical justification, unauthorized signatures (such as medical assistants or administrative staff), or failure to document bed-confinement status for stretcher requests. Only authorized clinicians—MDs, DOs, NPs, PAs, or CNSs—may sign these forms.
Step 3: Contact and Schedule an NEMT Provider
Once the assessment and documentation are complete, providers or their discharge/care coordination staff contact an approved NEMT company. This can be done directly with a licensed provider or through a Medicaid broker, depending on the patient's insurance. The scheduler must provide:
- Pickup address and destination
- Appointment time
- Special equipment needs (oxygen, bariatric equipment, stair assist)
- Round-trip or one-way service
Most programs require 24–72 hours advance notice. Florida's Medicaid broker MTM, for example, requires 3 business days for routine trips but offers 24/7 urgent scheduling within 3 hours for hospital discharges. Short-notice requests are reviewed case-by-case and may require additional justification.
When selecting a Florida NEMT provider, look for credentials that matter: 24/7 availability, PASS certification for wheelchair and stretcher transport, and staff who have passed background checks and DOT physicals. AllCare Medical Transport, based in Palm Coast, meets these requirements and works directly with healthcare facilities across Flagler, Alachua, and surrounding counties.
Step 4: Confirm the Pickup and Patient Handoff
Healthcare staff should confirm the pickup time with both the patient and the transport provider before discharge. Verify that the appropriate vehicle type is assigned and matches the PCS modality. For discharge situations, ensure a proper handoff:
- Confirm the patient's receiving location
- Provide any post-transport care instructions
- Identify who will receive the patient at the destination
- Document any special handling requirements (fall risk, oxygen dependency)
Step 5: Document and Follow Up
The final step covers documentation and follow-up. Facilities should:
- Confirm trip completion
- Flag any no-shows or transport failures for follow-up
- Keep transport records on file for compliance and quality review
- For recurring appointments (dialysis, chemotherapy), establish standing transport schedules and reassess modality whenever the patient's functional status changes
Key Factors That Affect the NEMT Process in Healthcare Settings
- Reassess transport modality when a patient's condition changes — after surgery, a fall, or a new diagnosis. PCS documentation must be updated whenever functional status shifts, not just at initial authorization.
- Medicaid, Medicare Advantage, and private insurers each carry different documentation requirements, prior authorization thresholds, and approved provider networks — staff coordinating NEMT must verify which rules apply to each patient's coverage.
- Rural and suburban patients often face fewer provider options, longer lead times, and limited vehicle types — especially for facilities in Florida counties like Flagler or Alachua, where specialized transport options are fewer than in major metro areas.
- Most NEMT programs require 3–5 business days for standard requests. Same-day discharges or urgent provider-scheduled appointments require escalation and will typically be denied without documented clinical justification.
- Verify that NEMT partners are licensed, fully insured (commercial and general liability), conduct driver background checks and drug testing, and hold CPR/First Aid and PASS certifications. Non-compliant vendors create direct liability for both the patient and the facility.

Common Misconceptions Healthcare Providers Have About NEMT
Misconception 1: "Any transport will do"
Many healthcare staff assume rideshare apps or family-arranged transport are acceptable substitutes for NEMT. For Medicaid patients, unauthorized transport may not be reimbursable. For patients with mobility or medical needs, non-credentialed transport creates real safety and liability risks.
Licensed NEMT providers address those risks through:
- Trained, background-screened drivers
- Proper equipment and securement systems
- Appropriate commercial insurance coverage
- Drug testing and DOT physical compliance
Misconception 2: "NEMT is the patient's responsibility to arrange"
For many patient populations—particularly hospital discharge patients and Medicaid beneficiaries—the healthcare provider or facility is expected to initiate or facilitate the NEMT request. Discharge planners who leave this to patients often see them arrive home without a ride—or miss critical follow-up appointments.
Proactive coordination by facility staff is both a quality-of-care issue and, in some cases, a regulatory expectation.
Misconception 3: "One transport type fits all patients"
The wrong transport modality is a common and consequential mismatch. Ordering ambulatory transport for a patient who needs a wheelchair van, or wheelchair transport for a patient who must lie flat, creates safety risks and may result in the transport being turned away at pickup—wasting time, delaying care, and triggering authorization issues. Clinical assessment must drive modality selection, and documentation must reflect the patient's true functional status.

Frequently Asked Questions
How much does non-emergency medical transport cost per hour?
NEMT is priced by vehicle type, distance, and service level — not a flat hourly rate. Ambulatory rides are the most affordable, with stretcher transport at the premium end; California's Medi-Cal schedule, for example, ranges from $17.65 for ambulatory to $26.29 base for stretcher vans. Rates also vary by region, time of day, and Medicaid versus private-pay status.
Will insurance cover non-emergency medical transportation?
Medicaid covers NEMT as a mandatory benefit in most states for eligible patients who have no other transportation option. Medicare generally does not cover routine NEMT, except in limited cases where strict bed-confinement criteria are met. Some Medicare Advantage plans include transport benefits as Special Supplemental Benefits for the Chronically Ill (SSBCI). Private insurance coverage is rare, and many patients use private pay for guaranteed availability and service quality.
How does NEMT differ from BLS?
Basic Life Support (BLS) transport is a level of emergency medical transport staffed by trained EMTs with on-board medical equipment for patients who are medically unstable or require monitoring during transit. NEMT is for medically stable patients who need assistance getting to a scheduled appointment but do not require clinical intervention during the ride. Ordering a BLS ambulance for a stable patient who only needs a stretcher van will result in claim denials.
What does ambulatory transportation mean?
Ambulatory transport refers to NEMT for patients who can walk independently or with minimal assistance (such as a cane or walker) and do not require a wheelchair or stretcher. These rides typically use standard sedans or vans and represent the most cost-effective tier of NEMT service. Patients must be able to transfer into and out of the vehicle safely with driver assistance.
How do healthcare facilities coordinate NEMT for discharged patients?
Discharge coordinators or social workers assess transport needs, complete required documentation (such as a Provider Certification Statement for Medicaid patients), and confirm pickup details with an approved NEMT provider before the patient leaves the facility. For non-Medicaid patients, staff typically provide referrals to licensed private NEMT companies and assist with scheduling.
What documentation does a healthcare provider need to arrange NEMT?
For Medicaid patients, a Provider Certification Statement (PCS) completed by a licensed practitioner is required, documenting functional limitations, transport modality, and clinical justification for why the patient cannot use public or personal transportation. For private-pay arrangements, providers need the pickup and destination addresses, appointment time, and any special equipment requirements.


