
Introduction
Transporting a patient over long distances—whether across Florida or across the country—is rarely as simple as booking a ride. The wrong choice of transport mode, missing documentation, or a poorly vetted provider can put a vulnerable patient at serious risk. For families and care coordinators managing hospital discharges, facility transfers, or relocations, the decisions come fast: Which transport mode is medically appropriate? What does the patient actually need during the journey? What will insurance cover?
Getting it wrong carries real consequences — especially when you're coordinating care for an elderly family member post-surgery, a dialysis patient moving closer to family, or a stroke survivor transferring to a specialized rehabilitation facility.
According to industry data, the U.S. Non-Emergency Medical Transportation (NEMT) market facilitates approximately 200 million trips annually, yet gaps in documentation, unclear medical needs, or rushed provider selection routinely derail even well-intentioned plans.
What follows is a practical breakdown of transport options, planning steps, and the factors that separate a safe, smooth journey from one that creates dangerous complications mid-trip.
TL;DR
- Long-distance patient transport is for non-emergency situations where a patient needs assisted travel over extended distances. It is not a substitute for 911.
- The right transport mode depends on medical condition, mobility level, distance, and budget. Common options include ground NEMT, air ambulance, and commercial escort.
- Start with physician sign-off confirming the patient is stable for transport and document all active care needs.
- Gather medical records, physician clearance, insurance information, and medication lists before booking.
- Vet providers on licensing, staff certifications (CPR/First Aid, PASS wheelchair and stretcher certification), vehicle equipment, and 24/7 availabilitybefore comparing prices.
Types of Long-Distance Patient Transport
Not all long-distance patient transport looks the same. The right method depends on the patient's condition, distance, urgency, and budget — choosing the wrong mode creates safety risks or unnecessary expense.
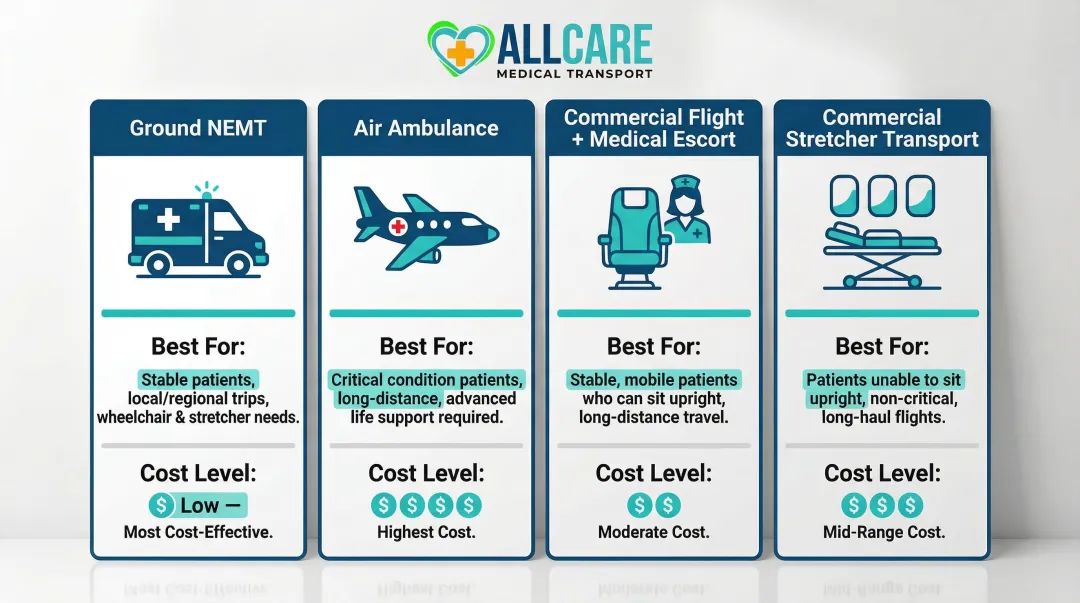
Ground Non-Emergency Medical Transport (NEMT)
Ground NEMT is the most common option for non-ambulatory, wheelchair-bound, or stretcher-dependent patients traveling hundreds or even thousands of miles. A trained attendant accompanies the patient for the full journey.
Vehicles are equipped with ramps, lifts, stretcher mounts, and basic medical support equipment to handle most non-critical transport needs.
This mode is generally the most cost-effective long-distance option and is appropriate when:
- The patient is medically stable
- No in-flight interventions are required
- The patient can tolerate travel time over hours or days
- Basic medical monitoring (oxygen, medication administration) is sufficient
AllCare Medical Transport is a PASS-certified NEMT provider based in Florida that handles this type of planned, long-distance ground transport — including wheelchair and stretcher trips across state lines or cross-country.
Air Ambulance
Air ambulance is the highest-acuity long-distance option — a fully equipped aircraft staffed by paramedics or flight nurses. Use this mode when:
- The patient is in critical or serious condition
- Advanced life support is needed during transit
- The patient must cover very long distances in minimal time
- Ground transport would take too long given the patient's medical urgency
Medicare's 2024 fixed-wing air ambulance base rate is $3,697.17 plus $10.50 per mile, making this the most expensive option. Private retail rates often exceed these amounts significantly.
Commercial Flight with Medical Escort
For medically stable patients who can tolerate a commercial flight, a trained medical escort (nurse or paramedic) accompanies the patient on a standard commercial airline. This is a cost-effective alternative to air ambulance for:
- Patients mobile enough to occupy a seat
- Elderly patients with cognitive or moderate physical limitations
- Patients who need supervision but not advanced life support
- Situations where time is important but not critical
Commercial Stretcher Transport
This hybrid air option installs a medical stretcher in the economy cabin of a commercial flight for patients who cannot sit upright but do not need a full air ambulance. A medical team travels alongside — significantly cheaper than a private air ambulance while still providing a higher level of in-flight care than a simple escort.
How to Arrange Long-Distance Patient Transport: Step by Step
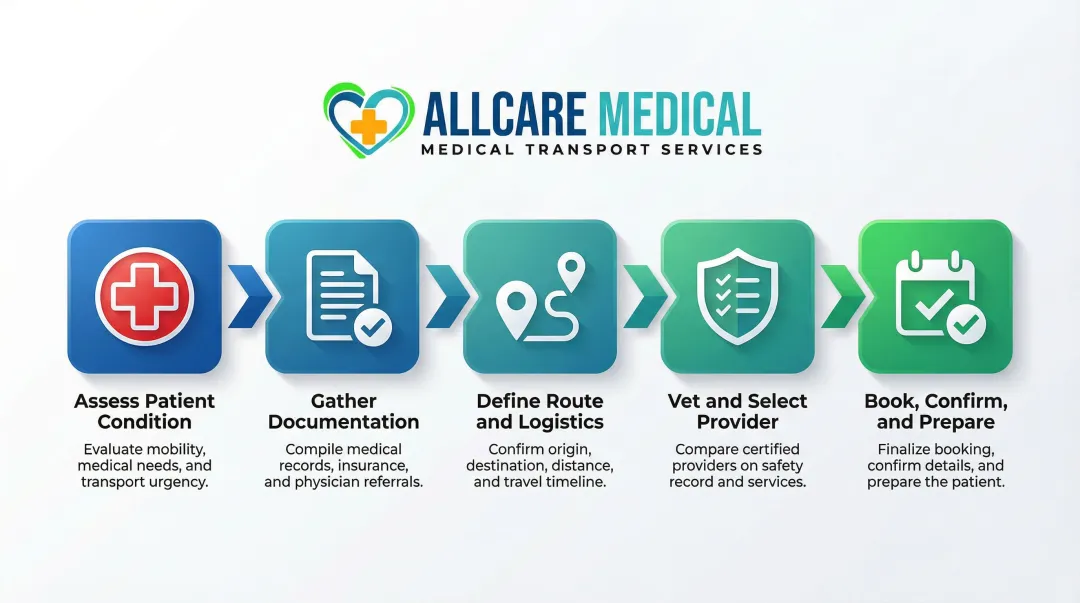
Step 1: Assess the Patient's Condition and Transport Eligibility
Confirm with the patient's physician or care team that the patient is stable enough for non-emergency long-distance transport. The doctor must determine:
- The journey will not worsen the patient's condition
- Any active care needs that must be maintained during transit (oxygen, feeding tube, medication schedule, repositioning schedule)
- Whether specific transport modes are ruled out — for example, flying may not be safe for patients with certain respiratory conditions
This assessment determines which transport mode is appropriate and what level of staffing and equipment the transport vehicle must have. For Medicare coverage, the physician must complete a Physician Certification Statement (PCS) confirming medical necessity.
Step 2: Gather All Required Documentation
Compile these documents before contacting any transport provider:
- Physician's sign-off letter or medical clearance
- Current medication list with dosing schedule
- Relevant medical records (diagnoses, recent treatment notes, imaging if relevant)
- Insurance cards and policy details
- Patient's DNR or advance directive if applicable
Incomplete documentation is a leading cause of booking delays and day-of complications. Having everything organized upfront lets the provider confirm they can meet the patient's needs — and helps avoid a refused transport at pickup.
Step 3: Define the Logistics and Scope of the Journey
Establish the full route details:
- Pick-up address: Home, hospital, or facility name and exact location
- Destination address: Receiving facility, home, or other location
- Estimated travel time: Account for distance and potential stops
- Required stops: Very long ground transports may need planned rest stops or overnight stays
Clarify the direction of the move — whether the patient is leaving a hospital for another facility, returning home from a care setting, or heading into one for the first time. Each scenario carries different handoff requirements at both ends of the trip.
Step 4: Research and Vet Transport Providers
Look for these qualifications when evaluating a provider:
Required Credentials:
- State licensing and insurance (commercial and general liability)
- Staff certifications (CPR/First Aid, PASS certification for stretcher/wheelchair transport)
- Background-checked and drug-tested employees
- DOT physical compliance for drivers
Beyond credentials, verify what the provider can actually deliver operationally:
- Vehicle type and equipment matching the patient's specific needs
- 24/7 availability for emergencies or schedule changes
- Clear communication policies so family stays updated during transit
- Ability to cover the full route, including cross-state trips
Ask whether the provider uses direct employees or subcontractors, since that directly affects accountability and consistency of care throughout the journey.
Step 5: Book, Confirm, and Prepare for Day of Transport
Walk through the booking confirmation process:
- Share all gathered documentation with the provider upfront
- Confirm the exact pick-up time and any required patient preparation — fasting, catheter status, or positioning needs
- Designate a family point of contact who will receive updates throughout the trip
- Pack essentials: Enough medication for the full trip plus extra, comfort items, copies of medical documents, and contact information for both sending and receiving care teams
What You Need Before Arranging Long-Distance Transport
Preparation directly affects both safety and logistics. Gaps in documentation, unclear medical needs, or an unprepared patient can compromise even a well-planned transport.
Patient Medical Readiness
The patient's physician must confirm:
- Current diagnoses and overall stability
- Active care needs during transit (oxygen flow rate, medication timing, turning schedule)
- Any contraindications to specific transport modes
- Medical necessity justifying the transport method selected
For Medicare coverage, the patient must meet strict "bed-confined" criteria: unable to get up from bed without assistance, unable to ambulate, AND unable to sit in a chair or wheelchair.
Documentation and Administrative Requirements
Required paperwork includes:
- Physician clearance letter
- Medication list with dosing schedule
- Insurance information and pre-authorization (if required)
- Medical records summary
- Advance directive or DNR
- Formal transfer order (for facility-to-facility transfers)
Provider Qualification Checklist
A qualified provider must have:
- Valid state transport license
- Appropriate vehicle for the patient's mobility needs (wheelchair van vs. stretcher-equipped vehicle)
- Certified and trained staff with documented credentials
- Liability insurance covering the full route
- Clear communication protocol with the patient's family
Insurance and Cost Preparation
Contact your insurer before booking to confirm coverage. Key rules to know:
- Medicare Part B covers non-emergency transport only if any other method would endanger the patient's health
- RSNAT prior authorization is required for 3 or more round trips within a 10-day period
- Medicaid varies by state — base rates and pre-authorization rules differ significantly
- Always request written pre-authorization confirmation before the transport date

Key Factors That Affect Your Long-Distance Transport Plan
Even with the right transport mode and a good provider, outcomes vary based on variables that families and care coordinators can anticipate and control.
Patient Condition and Care Needs During Transit
The complexity of ongoing care needs—supplemental oxygen, feeding tube, scheduled medications, cognitive monitoring—directly determines staffing requirements and vehicle equipment. A provider who isn't briefed on every active need before departure may lack the staff training or equipment to handle a situation once you're already on the road.
Critical questions to ask the provider:
- Can your vehicle accommodate oxygen tanks or concentrators?
- Is your staff trained to administer medications or manage feeding tubes?
- How do you handle repositioning or toileting needs during long trips?
- What happens if the patient's condition changes during transport?
The provider must be briefed on every active care need so they can confirm their staff and equipment can meet them before accepting the booking.
Distance and Route Planning
Cross-country ground transports may require planned rest stops, overnight stays, or driver rotation to ensure safety. Federal Motor Carrier Safety Administration (FMCSA) Hours-of-Service regulations (49 CFR Part 395) cap driving at 10 hours following 8 hours off-duty for passenger-carrying commercial vehicles weighing over 10,001 lbs or designed to transport 9+ passengers.
What to ask providers about long-haul logistics:
- How do you manage driver fatigue on multi-day trips?
- Are rest stops or overnight accommodations included in the quote?
- Do you rotate drivers, or does one driver complete the entire journey?
- What is your contingency plan if weather or traffic causes delays?
Provider Experience and Credentials
The logistics complexity of a long trip makes provider credentials non-negotiable. Before booking, verify:
- Asking for copies of state licenses and insurance certificates
- Confirming staff certifications (CPR, PASS) are current
- Checking online reviews and complaints with state regulatory agencies
- Requesting references from hospitals or facilities they've served
A provider who passes these checks has already demonstrated the accountability that protects your patient when plans change mid-route.
Common Mistakes When Arranging Long-Distance Patient Transport
Skipping Physician Clearance
Booking transport before confirming the patient is medically stable for travel—especially post-surgery or acutely ill patients—can result in serious deterioration during the journey or a provider refusing transport at pickup. Always obtain physician sign-off first.
Choosing a Transport Mode Based on Cost Alone
Selecting the cheapest option without matching it to the patient's actual condition and care needs creates safety risks. Using a basic wheelchair van for a patient who needs stretcher transport with oxygen may require a costly emergency response mid-trip and puts the patient in danger.
Failing to Communicate Care Needs to the Provider in Advance
Not disclosing the patient's full medical situation—active medications, positioning requirements, cognitive status—means the provider may arrive without the right equipment or staff training to support the patient safely. Share every detail upfront: a missed disclosure about a positioning requirement or cognitive condition can delay departure, trigger an equipment change, or create a safety gap mid-trip.
Avoiding these mistakes comes down to preparation. Before booking any long-distance transport, confirm medical clearance, match the transport mode to the patient's needs, and give the provider a full picture of the patient's condition.
Frequently Asked Questions
How much does long distance medical transport cost?
Costs vary widely based on mode, distance, and care requirements. Medicare reimburses ground ambulance at approximately $272.44 base rate plus $8.76 per mile for 2024, though private retail rates differ. Air ambulance is significantly more expensive, often exceeding $30,000 for long-distance flights.
What are the different ways to transport a patient long distance?
The main options are ground NEMT (wheelchair/stretcher), air ambulance, commercial flight with medical escort, and commercial stretcher transport. The right method depends on the patient's medical condition, distance, and whether they can tolerate standard seating or require specialized positioning and monitoring.
Does Medicare cover long distance transportation?
Medicare Part B covers non-emergency ambulance transport only when other transportation methods could endanger the patient's health. Pre-authorization is required for repetitive scheduled transports (3+ round trips in 10 days), and your physician must thoroughly document medical necessity to support the claim.
How to transport an elderly person across country?
Get physician clearance first, then assess mobility and care needs to choose between ground NEMT or air options. Book a licensed provider in advance with documentation ready — medication lists, medical records, and insurance pre-authorization if required.
What to do if you have no one to drive you home from the hospital?
Licensed NEMT providers like AllCare Medical Transport offer hospital discharge transport for patients who cannot arrange a personal ride. Hospitals can often help coordinate this referral, and some insurance plans may cover the cost. AllCare is available 24/7 — reach them at 386-864-7145 or through your hospital's discharge coordinator.
How far in advance should I book long-distance medical transport?
Ideally, book at least 5-7 days in advance for planned transports to allow time to gather documentation and confirm logistics. Reputable providers with 24/7 availability can accommodate shorter notice, but earlier booking reduces stress and ensures vehicle and staff availability for your preferred date.


