Introduction
Picture this: Maria, a 72-year-old Palm Coast resident with diabetes, sits at home holding her insulin prescription. Her pharmacy is only four miles away, but it might as well be forty. She doesn't drive anymore, the local bus stop is a 15-minute walk she can't manage with her walker, and her daughter works full-time an hour away. Today, Maria will skip her refill. Tomorrow, her blood sugar will climb. Next week, she might end up in the emergency room.
Maria's story isn't unique—it's a silent health crisis affecting millions of Americans. According to the CDC, 5.7% of U.S. adults lack reliable transportation for daily living, and an estimated 5.8 million individuals delayed medical care in 2017 due to transportation barriers. The CDC and HHS Healthy People 2030 officially recognize transportation as a Social Determinant of Health—a fundamental factor that shapes health outcomes and access to care.
When patients can't reach their pharmacy, the consequences pile up fast: missed medications worsen chronic conditions like hypertension and diabetes, preventable hospitalizations strain the healthcare system, and emergency care use spikes.
Understanding what drives these gaps—and what actually solves them—is the focus of this article. It covers the types of barriers blocking medication access, who faces the greatest risk, and practical solutions ranging from trip planning strategies to professional transportation options like non-emergency medical transport (NEMT).
TLDR: Key Takeaways
- Transportation barriers include cost, unreliable services, long distances, and coordination failures
- Seniors, low-income individuals, people with disabilities, and rural residents face the highest risk
- Missed medications directly worsen chronic disease outcomes and increase emergency care use
- Solutions include trip chaining, mail-order pharmacy, telehealth, and professional NEMT services
What Are Transportation Barriers to Medication Access?
Transportation barriers are any obstacles preventing patients from physically reaching a pharmacy, medical appointment, or medication pickup. These obstacles include common issues like not owning a car or living far from the nearest pharmacy, alongside subtler problems like unreliable paratransit schedules, expensive ride-share fees, or dispatch failures that leave patients stranded.
Research reveals the scope: an estimated 3.6 million Americans miss at least one medical trip annually because of transportation issues. For patients managing chronic conditions requiring regular medication refills—diabetes, hypertension, heart disease—these barriers aren't just inconvenient. They're dangerous.
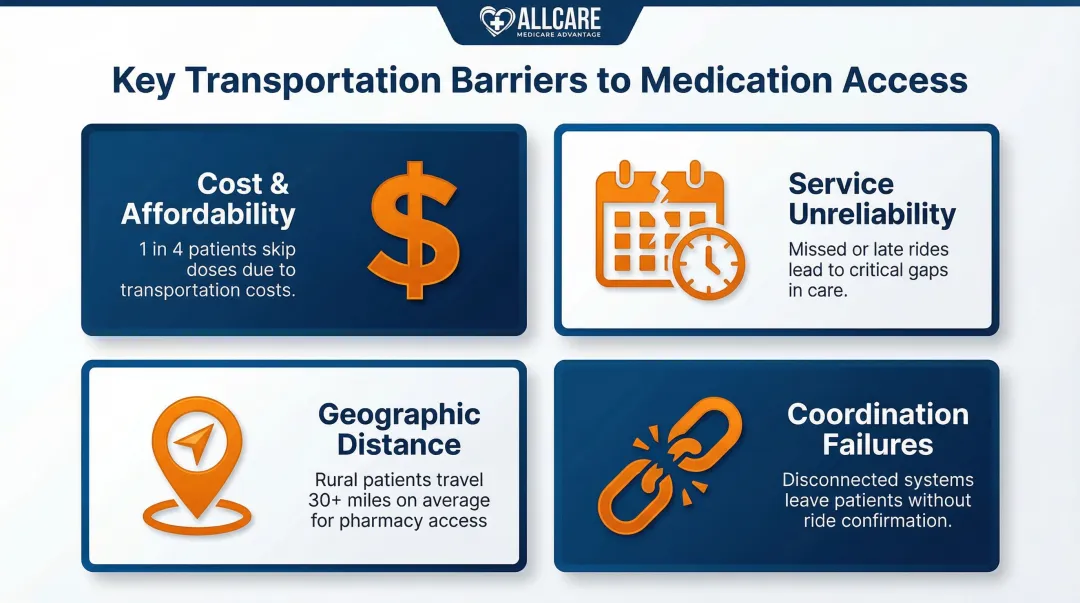
Specific Barrier Types
Cost and Affordability
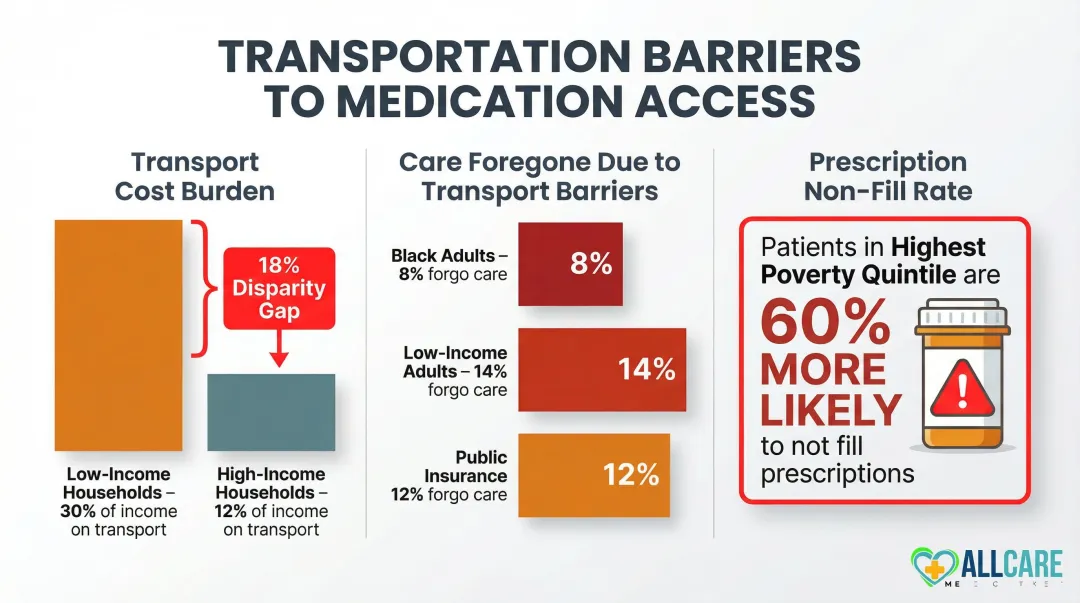
Even when transportation exists, it's often financially out of reach. The lowest-income households spend 30% of their after-tax income on transportation, compared to 12% for high-income households.
For patients on Social Security or Medicaid—of whom 20.4% report lacking reliable transportation—bus fares, gas, ride-share fees, and parking add up fast. When the choice is between groceries and a $15 Uber to pick up insulin or blood pressure medication, medication access loses.
Wait Times and Service Unreliability
Long waits for paratransit, missed pickups, and dispatch coordination failures sabotage medication schedules. A 2021-2023 audit of Chicago's ADA Paratransit revealed on-time drop-off rates of just 84.06%—falling short of the 90% internal target. When a ride scheduled for 2:00 PM arrives at 4:30 PM, patients miss pharmacy closing times, medication windows, and appointments.
This unreliability erodes trust. Patients who've been stranded once are less likely to schedule future trips, creating a cycle of disengagement from care.
Geographic and Physical Access
Distance is a growing problem. Between 2010 and 2021, 29.4% of U.S. retail pharmacies closed, creating pharmacy deserts where 15.8 million Americans—including over 749,000 Floridians—face significant travel distances to reach a pharmacy.
In areas like Flagler County or Palm Coast, limited public transit means car ownership or dedicated transport services are essential, not optional. Patients using walkers, canes, or recovering from surgery face the additional challenge of managing the physical trip itself and carrying medications home.
Systemic Coordination Failures
Communication breakdowns between dispatchers, drivers, and patients plague NEMT and insurance-provided transport. HHS-OIG audits of Medicaid NEMT programs found significant non-compliance—including lack of documentation proving services were actually provided or that drivers met credential requirements. Rides are scheduled but don't arrive, leaving patients stranded and appointments missed.
Who Is Most at Risk?
Seniors and people with disabilities
Older adults and individuals with mobility limitations face compounding transportation barriers. Among Medicare beneficiaries, 17.4% report trouble getting to places like the doctor's office, with significantly higher odds for those aged 85+ and those with dual Medicaid eligibility.
For this group, those barriers tend to compound:
- Loss of driving ability — often permanent
- Higher pharmacy visit frequency for multiple chronic conditions
- Physical inability to use standard transit (buses, trains, ride-shares without accessibility features)
- Greater reliance on specialized transport services that may not always be available
These access gaps carry consequences that reach well past missed prescriptions. Driving cessation in older adults almost doubles the risk of increased depressive symptoms and nearly quintuples the likelihood of admission to long-term care facilities.
Low-income individuals managing chronic conditions
Patients with diabetes, hypertension, and heart disease must access medications on a regular, non-negotiable schedule. Transportation disruptions for this population directly compromise disease management. Research shows that one-third of adults with Medicaid who are in fair or poor health lacked reliable transportation in the past 12 months.
The prescription data reinforces this. A regional pharmacy chain study found that nearly 1 in 8 pediatric prescriptions went unfilled — and 1 in 4 of those were in high-poverty, low-vehicle zip codes. Income and access gaps overlap in clear patterns:
- Patients in the highest poverty quintile were 60% more likely to not fill prescriptions than those in low-poverty areas
- Black adults (8%), adults with low family incomes (14%), and adults with public health insurance (12%) were more likely to forgo care entirely due to transportation difficulty
Rural and suburban residents
Patients in areas like Flagler County or Palm Coast face fewer public transit options and greater distances to pharmacies. Florida alone has 749,103 adults living in pharmacy deserts. In nonmetropolitan pharmacy desert counties, residents must drive an average of 85 minutes to reach a pharmacy.
For residents without a car or access to reliable NEMT services, that 85-minute drive isn't a minor inconvenience — it's a barrier that often means going without. This is exactly the gap that dedicated medical transportation is designed to close.
How Transportation Barriers Affect Medication Adherence and Health
Missed and delayed prescription fills
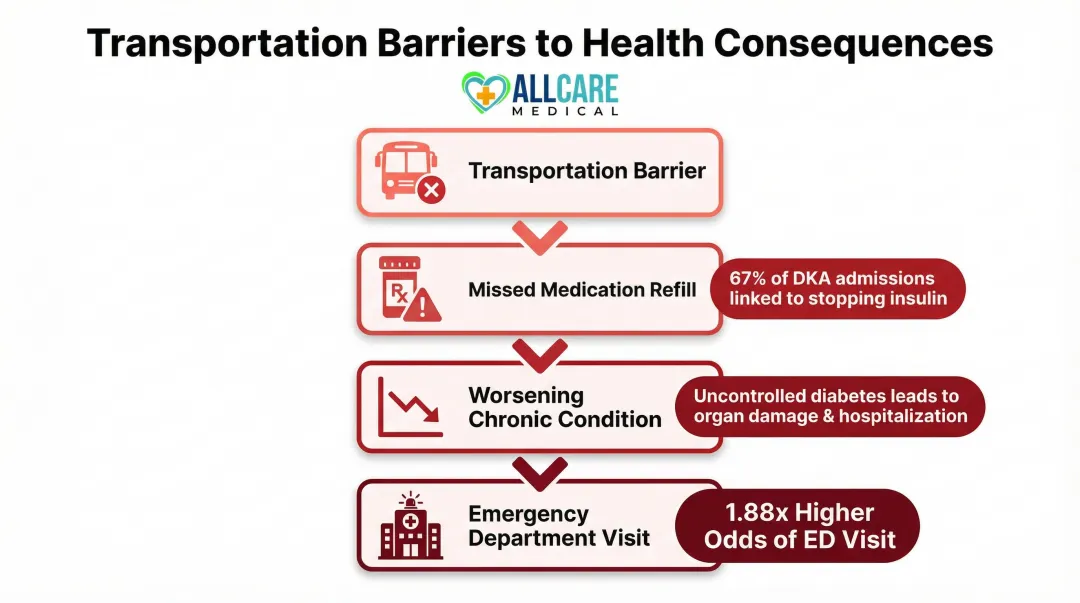
When patients can't get to a pharmacy, they delay or skip refills. Research on diabetic ketoacidosis (DKA) admissions found that 67% were related to stopping insulin, and 50% of those patients cited either lack of money for insulin or lack of transportation to get their medicine.
Following hospital discharge, patients reporting difficulty visiting the pharmacy had significantly lower prescription fill rates than those not reporting difficulty—20% versus 55%. A cohort study of Medicaid patients found that restricting Medicaid payments for transportation resulted in an 18% decline in visits for medication refills.
Worsening chronic disease management
Skipped medications lead to uncontrolled blood pressure, blood sugar spikes, and pain flare-ups. Each missed dose compounds over time for conditions requiring consistent schedules. Pharmacy closures trigger immediate 5.6% to 5.9% absolute declines in adherence to cardiovascular medications among older adults—including statins and beta-blockers that prevent heart attacks and strokes.
For patients with diabetes, hypertension, or cardiac disease, transportation-driven medication gaps translate directly into disease progression and complications.
Increased emergency care and hospitalizations
Transportation barriers increase the likelihood of ED visits. Adults with at least one access barrier had 1.88 times higher odds of an ED visit in a one-year period. Among younger adults (18-64), patient-reported delayed care due to transportation barriers is associated with increased odds of ED use—1.47 times for hypertension, 1.50 times for cardiac disease, and 1.50 times for diabetes.
Most of these visits are preventable: patients who miss routine refills experience acute exacerbations—diabetic crises, hypertensive emergencies, heart failure episodes—that escalate into emergency interventions.
Emotional and psychological toll
Transportation barriers erode mental health and trust in healthcare alongside the physical consequences. Patients describe anxiety, frustration, and helplessness when they can't reliably access their own medications. The emotional weight shows up in the logistics too:
- Paratransit scheduling difficulties and extended wait times add physical strain on top of the stress
- Rides lasting 2 to 3 hours for a simple pharmacy pickup are not uncommon
- Repeated friction causes patients to disengage from care entirely
The appointment cascade
Missing a pharmacy pickup disrupts more than just that day's medication. It triggers a cascade of missed appointments:
- When the patient never picks up the prescription, a follow-up appointment gets canceled before it begins
- Rescheduling typically takes weeks or months for patients managing chronic conditions
- Each delay compounds the last, creating a cycle of deferred care that worsens outcomes and drives up costs
Practical Strategies Patients and Caregivers Can Use
Trip planning and batching
Cluster multiple errands into a single trip on the same day to minimize transportation costs and dependence. Combine:
- Pharmacy pickup
- Doctor's appointment
- Grocery shopping
- Lab work or diagnostic tests
Coordinating with a caregiver or family member in advance makes trip batching more feasible and reduces the number of individual rides needed throughout the month.
Using multiple transportation modes strategically
Match transport type to trip urgency and distance:
- Insurance-provided NEMT for scheduled medical appointments and specialty visits
- Ride-share services for urgent pharmacy pickups or same-day needs
- Senior county programs for grocery trips and non-medical errands
- Public transit for routine refills when mobility allows
Know eligibility requirements for each option in advance. Medicaid beneficiaries, for example, may qualify for NEMT but must confirm coverage and book ahead.
Leveraging social networks
Family, friends, neighbors, and peer support can fill transportation gaps when formal services fall short. These rides are often more flexible and affordable than commercial options, but require advance planning and may not be available for time-sensitive pickups. Identifying 2-3 people willing to rotate trips spreads the responsibility and keeps any one person from burning out.
Mail-order and delivery pharmacy programs
Mail-order pharmacy helps patients on maintenance medications cut down on in-person pharmacy trips significantly. Patients using mail-order pharmacies demonstrate 2.2 to 2.3 times higher odds of adhering to antidiabetic medications. A study of Medicare Advantage patients with diabetes found that mail-order pharmacy users maintained higher adherence through 48 months compared to community pharmacy users—78% versus 62%.
Key advantages:
- 90-day supply refills reduce the number of trips required from 12 per year to just 4
- Home delivery is associated with 23% to 32% fewer non-adherent individuals compared to retail 90-day fills
- Many insurance plans now offer home delivery at reduced or no cost

For patients who still need in-person appointments, telehealth can reduce how often those trips are required.
Telehealth and digital care management
Telehealth visits reduce the frequency of in-person appointments required for prescription renewals. However, overall telemedicine use among U.S. adults decreased from 37.0% in 2021 to 30.1% in 2022, and adoption barriers remain significant.
Challenges include:
- Digital literacy gaps among older adults
- Over 26% of Medicare beneficiaries lack computer or smartphone access at home
- 22.3% of Americans in rural areas lack fixed broadband access, compared to 1.5% in urban areas
Telehealth works best when combined with technical support from family members or "digital navigators" who help patients use the technology.
Systemic and Community Solutions
Healthcare and transportation coordination
Healthcare institutions can reduce barriers through:
- Offering transportation assistance programs or subsidies
- Partnering with ride-share platforms like Uber Health for on-demand transport
- Training staff—including "digital navigators"—to help patients understand and access available transport options
- Coordinating between schedulers, pharmacies, and transport providers to reduce dispatch failures
Better coordination prevents dispatch failures that leave patients stranded. When a hospital discharge team books a pharmacy pickup ride directly with an NEMT provider, the patient navigates one call instead of three.
Expanding NEMT coverage and community programs
Policy changes can reduce financial transportation barriers. From 2020 to 2024, 100% of Medicare Advantage Value-Based Insurance Design (VBID) plans offered NEMT, compared to 44.5% of traditional MA plans. VBID plans feature fewer restrictions—including unlimited trips and lower copays.
Community programs to expand:
- Medicaid NEMT benefits with broader pharmacy trip coverage
- County senior transportation programs with increased capacity
- Fare capping or trip limit expansions on public transit
- Subsidized ride-share vouchers for low-income patients
CMS guidance clarifies that if a state covers prescribed drugs, it must also assure beneficiaries have necessary transportation to pick up covered prescriptions. States may adopt policies to combine a return trip from a medical provider with a stop at the nearest participating pharmacy.
Peer-led and community transport models
Peer-led transportation programs—particularly in recovery, substance use treatment, and chronic care communities—build trust and reduce anxiety. Drivers with shared lived experience do more than transport patients:
- Provide emotional support during stressful medical visits
- Reduce isolation for patients managing long-term conditions
- Help patients stay consistently engaged with care over time
- Lower no-show rates by offering a reliable, non-judgmental presence
These models are especially effective for patients who have experienced trauma or stigma in healthcare settings. A familiar, trusted driver removes one more reason to skip an appointment.
When to Consider Professional Non-Emergency Medical Transportation (NEMT)
What NEMT is and who it serves
Non-emergency medical transportation is designed specifically for patients who need to reach medical appointments, pharmacy pickups, or treatment centers but cannot use standard transportation. NEMT serves patients in wheelchairs, on stretchers, or those who need attendant assistance boarding and exiting vehicles.
Unlike emergency ambulance services, NEMT is scheduled in advance for patients who require specialized transport but are medically stable.
Between 3 million and 4 million Medicaid beneficiaries used NEMT annually between 2018 and 2021. NEMT utilization is highest among beneficiaries with substantial health care needs, such as those with end-stage renal disease (ESRD), who averaged 5.5 monthly ride days per user in 2021.
A systematic review found that providing NEMT to patients with transportation barriers is associated with a significant reduction in missed clinic appointments (patients were 37% less likely to miss appointments).
Key scenarios where NEMT is the right choice
NEMT is especially appropriate for:
- Post-discharge pharmacy pickups after surgery or hospitalization
- Recurring specialist visits for dialysis, chemotherapy, or cardiac rehabilitation
- Patients with limited mobility who need boarding and exiting assistance
- Long-distance inter-facility transfers requiring comfort and safety
- Time-sensitive medication pickups that depend on reliable, scheduled transport
In Florida, AllCare Medical Transport provides 24/7 availability with CPR-certified, PASS-certified staff and wheelchair- and stretcher-equipped vehicles serving Flagler County, Palm Coast, Daytona, and surrounding areas.
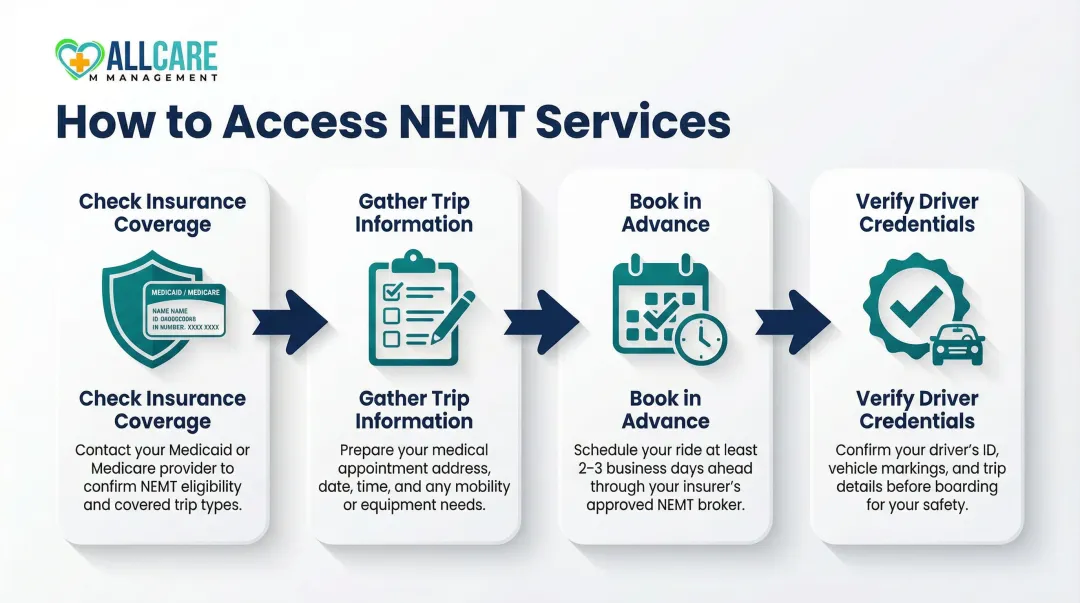
How to access NEMT services
Step 1: Check insurance or Medicaid coverage
- Contact your insurance plan or Medicaid managed care organization to confirm NEMT benefits
- Ask specifically if pharmacy pickups are covered (coverage varies by state and plan)
- Request documentation of coverage limits (trip frequency, distance, copays)
Step 2: Gather necessary information before booking
- Appointment date and time
- Pickup location (home address or current facility)
- Destination address (pharmacy, medical office, treatment center)
- Mobility needs (ambulatory, wheelchair, stretcher)
- Any special accommodations (oxygen, attendant, medical equipment)
Step 3: Book in advance
- Contact the NEMT provider as early as possible (ideally 24-48 hours before the trip)
- Provide all necessary information at booking
- Confirm pickup time and any wait time policies
Step 4: Verify credentials and safety protocolsAsk potential providers about:
- Driver certifications: CPR, First Aid, PASS (wheelchair/stretcher transport)
- Background checks and drug testing policies
- Vehicle inspection and maintenance records
- Insurance coverage: commercial and general liability
- 24/7 availability and backup vehicle policies
For patients in Palm Coast and surrounding areas, AllCare Medical Transport can be reached at (386) 864-7145 for free quotes and booking assistance.
Frequently Asked Questions
What are the most common transportation barriers to picking up medications?
The most common barriers include:
- Cost: bus fares, gas, and parking fees strain fixed incomes
- Unreliable services: paratransit failures, missed rides, or no-shows
- Distance: rural and suburban areas often lack public transit routes near pharmacies
- Mobility limitations: standard transport isn't accessible for many patients
- Coordination failures: rides get scheduled but drivers don't arrive
Does Medicare or Medicaid cover transportation to the pharmacy?
Medicaid typically covers NEMT for medical appointments, and CMS guidance requires states that cover prescribed drugs to assure beneficiaries have necessary transportation to pick up prescriptions—though coverage varies by state and plan. Traditional Medicare (FFS) does not cover routine non-emergency transportation, only ambulance services when other transport could endanger health. Check your specific plan benefits and ask your care coordinator about eligibility.
What is non-emergency medical transportation (NEMT) and who qualifies?
NEMT provides scheduled transport for patients who need help reaching medical appointments or pharmacy pickups but don't require emergency ambulance care—including wheelchair users, stretcher patients, and those needing boarding assistance. Medicaid beneficiaries typically qualify when they lack other transportation means; some Medicare Advantage plans offer NEMT benefits as well.
How can seniors without a car get to their pharmacy or medical appointments?
Several options are available:
- Insurance-provided NEMT (check Medicaid or Medicare Advantage coverage)
- County senior transportation programs, often subsidized
- Healthcare ride-share platforms (Uber Health, Lyft)
- Mail-order pharmacy delivery for 90-day supplies
- Family, volunteer networks, or your local Area Agency on Aging
Can a medical transport service take me to a pharmacy, not just a doctor's office?
Yes, many NEMT providers transport patients to pharmacies, treatment centers, dialysis facilities, and other medical destinations—not just physician offices. Confirm this scope of service when booking. AllCare Medical Transport, for example, provides transport to pharmacies, dialysis centers, and other healthcare destinations throughout Florida.
What should I do if I miss a medication pickup due to a transportation problem?
Call your prescribing physician or pharmacist to discuss options—many pharmacies have emergency refill policies for critical medications. Ask about mail delivery for future refills, and consider a telehealth consultation to manage any symptoms until transport is arranged.


